What are spider veins?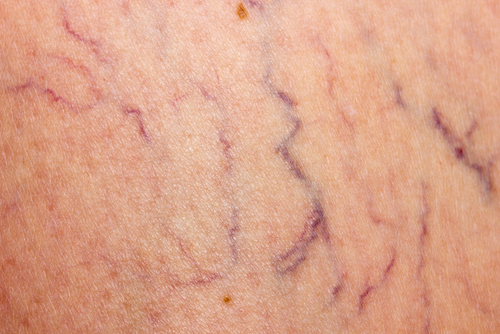
Small “spider veins” also can appear on the skin’s surface. These may look like short, fine lines, “starburst” clusters, or a web-like maze. Spider veins are most common in the thighs, ankles, and feet. They may also appear on the face.
Who gets varicose and spider veins?
Varicose and spider veins can occur in men or women of any age, but most frequently affect women of childbearing years and older. Family history can also increase the tendency to develop varicose and spider veins. What causes varicose and spider veins? The causes of varicose and spider veins are not entirely understood. In some instances, the absence or weakness of valves in the veins, which prevent the backward flow of blood away from the heart, may cause the poor circulation. In other cases, weaknesses in the vein walls may cause the pooling of the blood. Less commonly, varicose veins are caused by such diseases as phlebitis (inflammation of the veins) or congenital abnormalities of the veins. Venous disease is generally progressive and cannot be prevented entirely. However, in some cases, wearing support hosiery and maintaining normal weight and regular exercise may be beneficial.
Is treatment always necessary?
No. Varicose and spider veins may be primarily a cosmetic problem. Severe cases of varicose veins, especially those involving ulcers, typically require treatment. Thousands of people every year consider getting treatment for varicose veins and spider veins. Advertisements for treating venous disease often tout “unique,” “permanent,” “painless,” or “absolutely safe” methods – making it difficult to decide on the best treatment.What are varicose veins?
A vein is a blood vessel that carries blood low in oxygen content from the body to the lungs and heart. It is a normal part of the circulatory system. Veins can bulge with pools of blood when they fail to circulate the blood properly. These visible and bulging veins, called varicose veins, are often associated with symptoms such as tired, heavy, or aching limbs. In severe cases, varicose veins can rupture, or open sores (called “ulcers”) can form on the skin. Varicose veins are most common in the legs and thighs.
What procedures are available to treat varicose and spider veins?
Varicose veins are frequently treated by eliminating the “bad” veins. This forces the blood to flow through the remaining healthy veins. Various methods can be used to eliminate the problem veins, including, most commonly, surgery to close them down or remove them, or sclerotherapy (injection of irritating substances into the problem vein to irritate the vein lining and close them down). Less commonly, laser or electro-cautery treatments have been used to treat the smallest spider veins, especially on the face. Surgery to treat varicose veins, commonly referred to as “stripping,” is usually done under local or partial anesthesia, such as an epidural. Here, the problematic veins are “stripped” out by passing a flexible device through the vein and removing it through an incision near the groin. Smaller tributaries of these veins also are stripped with this device or removed through a series of small incisions. Those veins that connect to the deeper veins are then tied off. This stripping method has been used since the 1950s. Spider veins cannot be removed through surgery. Sometimes, they disappear when the larger varicose veins feeding the spider veins are removed.
Remaining spider veins also can be treated with sclerotherapy. Sclerotherapy uses a fine needle to inject a solution directly into the vein. This solution irritates the lining of the vein, causing it to swell and the blood to clot. The vein turns into scar tissue that fades from view. Some doctors treat both varicose and spider veins with sclerotherapy. Today, the substances most commonly used in the U.S. are hypertonic saline, sodium tetradecyl sulfate (Sotradecol) and aethoxysklerol/Asclera (Polidocanal). During sclerotherapy, after the solution is injected, the vein’s surrounding tissue is generally wrapped in compression bandages for several days, causing the vein walls to stick together. Patients whose legs have been treated are put on walking regimens, which forces the blood to flow into other veins and prevents blood clots. This method and variations of it have been used since the 1920s. In most cases, more than one treatment session will be required.